February 2020 Newsletter

For a list of food pantries and meal sites in Berkshire county, click HERE

BOAPC Receives 3-Year, $300,000 Grant to Develop Post-Overdose Engagement Program
We are happy to report that BOAPC has been awarded a grant from the Massachusetts Department of Public Health/Bureau of Substance Addiction Services to continue its essential work until FY 22. This funding originates as a CDC grant (Overdose Data to Action) that BSAS set-aside, in order to fund eligible coalitions for 3 additional years (as current MOAPC funding ends 6/30/2020). In partnership with Northern Berkshire Community Coalition, this grant’s goal is to fund BOAPC and community partners to focus on developing and implementing post-overdose engagement programs in the Northern Berkshire region, funding a 4-Western Massachusetts County Rural Opioid Data Collaborative (RODC), and to develop the Beacon Recovery Community Center (BRCC) to be a naloxone (Narcan) training/access point.
Congratulations to all involved in the efforts related to this successful grant application! We are excited to do this essential community work.

Estimating the impact of drug use on US mortality, 1999-2016
By: Dana A. Glei, Samuel H. Preston
“The impact of rising drug use on US mortality may extend beyond deaths coded as drug-related to include excess mortality from other causes affected by drug use. Here, we estimate the full extent of drug-associated mortality.”
https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0226732
Challenges in Providing Substance Use Disorder Treatment to Child Welfare Clients in Rural Communities
Authors: Elizabeth Clary, Christina Ribar, and Elizabeth Weigensberg
Project Officers: Laura Radel and Emily Madden
KEY FINDINGS
- Rural communities often lack the resources to provide services to parents struggling with substance use issues. Rural economics, transportation and technological limitations exacerbate these challenges.
- Child welfare agencies and substance use disorder treatment providers face particular challenges to collaboration with one another in rural communities. Stigma, lack of anonymity and misinformation compound these issues.
- Strategies specifically tailored to rural communities are needed to improve service access, develop workforce capacity and improve collaboration.

Feds to Let States Tap Opioid Funds for Meth, Cocaine Surge
By The Associated Press
“Alarmed by a deadly new twist in the nation’s drug addiction crisis, the government will allow states to use federal money earmarked for the opioid epidemic to help growing numbers of people struggling with meth and cocaine.”
https://www.nytimes.com/aponline/2020/01/21/us/politics/ap-us-drug-crisis-meth-and-cocaine.html
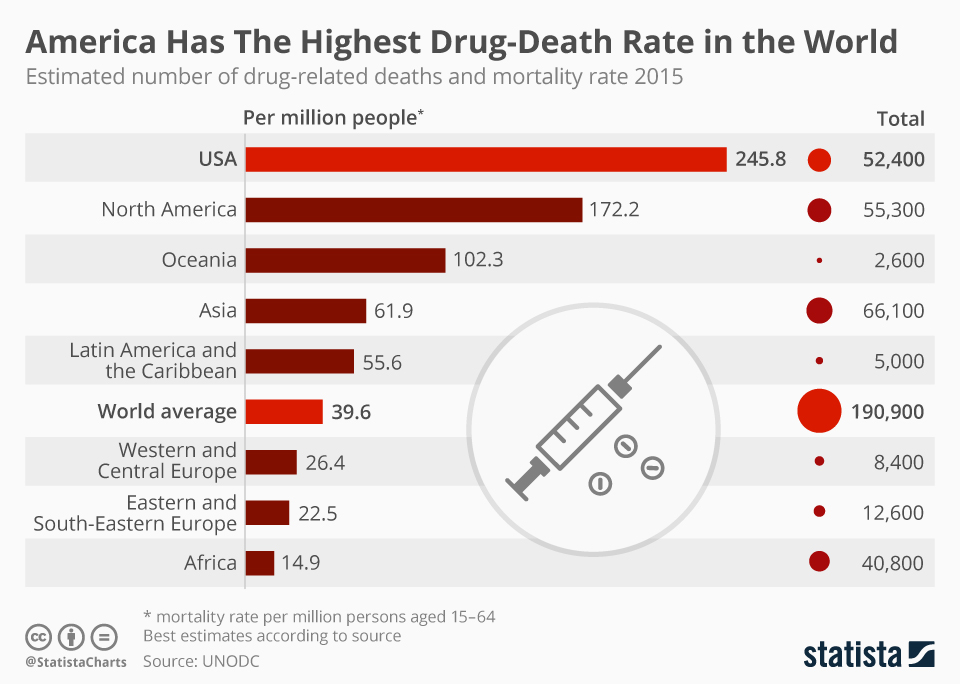
America leads the world in drug overdose deaths — by a lot
By German Lopez
“America has about 4 percent of the world’s population — but about 27 percent of the world’s drug overdose deaths.”
https://www.vox.com/policy-and-politics/2017/6/28/15881246/drug-overdose-deaths-world
New federal program hopes to prevent homelessness in young adults aging out of foster care system
By Daniel Langhorne
“Giggling with excitement, Christian, a 22-year-old former foster youth, showed off his new apartment in Tustin on Thursday.”
https://www.latimes.com/california/story/2019-12-23/federal-foster-program-homeless

‘Like A Flu Shot’ For Addiction Crisis — Training High School Students As Recovery Coaches
By: Kara Leigh Lofton
“In Clay, downtown Main Street is maybe a half mile long. Amid shuttered storefronts, the two most prominent stores are Family Dollar and the Dollar Tree. Like the rest of southern West Virginia, the opioid epidemic has hit Clay hard. “I would venture to guess that every single student in this entire school has been affected by addiction in some way,” said Leslie Osborne, the school counselor.”
https://www.wvpublic.org/post/flu-shot-addiction-crisis-training-high-school-students-recovery-coaches#stream/0
Employer Resource Library
“The Grayken Center for Addiction at Boston Medical Center (BMC) has designed a set of tools and resources to support your organization in understanding and addressing substance use disorders (SUDs). These tools are free to use, regardless of where or how your organization receives its medical care.”
https://www.bmc.org/addiction/employer-resource-library


Podcast: Integrating Reproductive Health Services into Opioid Treatment Facilities
“In episode fifteen of Addiction Medicine: Beyond the Abstract, we are joined by Dr. Tricia Wright, MD, MS, FACOG, DFASAM. She is a professor of clinical medicine at the University of California San Francisco. In her recent commentary, Dr. Wright discusses some of the challenges facing women in opioid treatment programs and the need for the provision of reproductive healthcare to this population.”
Why Boston Drug Users Are Wary of Emergency Medical Care
By: Filter Staff
“Wound care for people who inject drugs is considered a critical component of harm reduction by providers. But people who inject drugs (PWID) in Boston, Massachusetts hesitate to access medical care because of perceptions that the medical system will not meet their needs, found a study by Boston Medical Center (BMC). And drug user activists recently spoke out about their own experiences with the hospital.”
https://filtermag.org/boston-drug-users-emergency-care/amp/

Opportunities to Increase Screening and Treatment of Opioid Use Disorder Among Healthcare Professionals
Shatterproof, RIZE Massachusetts, and GE Foundation Release Survey on Massachusetts Healthcare Professionals and Stigma around Screening, Treating Patients with Opioid Use Disorder Research Finds that Stigma Around Addiction Extends to Provider Community
Key survey findings among respondents include:
- Only 1 in 4 providers had received training on addiction during medical education
- Only 1 in 10 EM providers found caring for patients with OUD satisfying
- Less than 50% of EM and FM/IM providers believed that OUD is treatable
- Almost one third of providers with more than 20 years of tenure tended to have a stronger preference for not working with patients with OUD.
- Almost half of providers felt patients would not be honest about their opioid use if asked directly
- Less than 1/3 of EM, OBGYN/Women’s Health, or pediatric providers feel very prepared to screen, diagnose, provide brief intervention for, or discuss or provide treatment for OUD
- 2x as many EM providers than any other specialty believe methadone treatment for OUD is substituting one addiction for another
- 2 in 5 EM or FM/IM providers feel that treating patients with OUD takes away time and resources from other patients
- More than 50% of Emergency Medicine, FM/IM, OBGYN/Women’s Health providers feel they don’t have sufficient access to behavioral health support to start patients on medication for addiction treatment.
https://rizema.org/wp-content/uploads/2019/07/GE-Rize-Shatterproof-White-Paper-Final.pdf

For more information about the Berkshire Opioid Addiction Prevention Collaborative, its partners, or to obtain a complete list of BOAPC activities and events, please contact [email protected].
This program in funded by the Massachusetts Department of Public Health Bureau of Substance Addiction Services.

